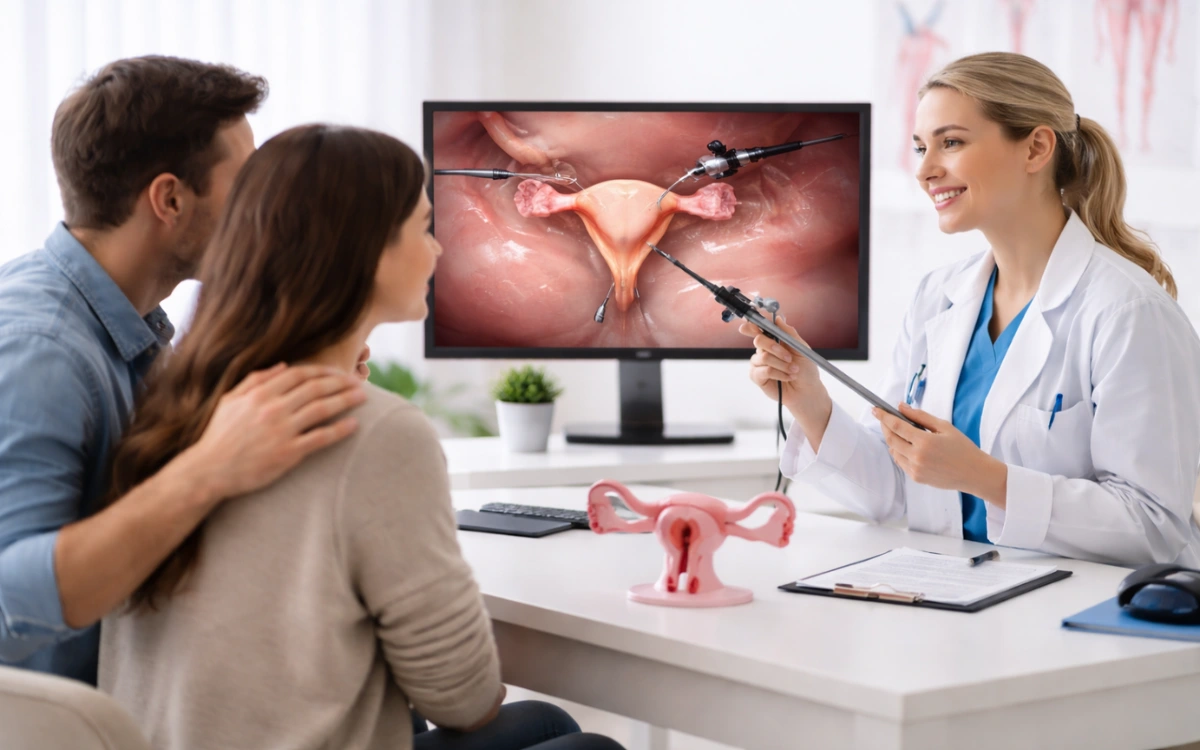
Many women exploring fertility care come across the option of laparoscopic surgery for fertility. This minimally invasive technique has become an important tool in modern reproductive medicine. It helps diagnose hidden problems, treat underlying conditions, and improve the chances of natural conception. For women who have been trying to conceive without success, laparoscopy often provides the clarity and treatment needed to move forward with confidence.
When fertility challenges feel uncertain or unexplained, the emotional weight can be heavy. You may be doing everything right, tracking cycles, eating well, and maintaining a healthy lifestyle, yet still not seeing the progress you hope for. Laparoscopy offers a closer look at your reproductive organs and helps identify issues that might not appear on routine scans or blood tests. Understanding how this procedure works gives you more control over your journey and helps you make informed decisions.
What Is Laparoscopy and Why Is It Used in Fertility Care?
Laparoscopy is a minimally invasive surgical procedure that allows your doctor to see inside your abdomen and pelvis using a small camera. When used as part of fertility evaluation, it helps identify structural issues that may affect conception.
Many conditions affecting fertility cannot be diagnosed clearly through ultrasound alone. This is where diagnostic laparoscopy fertility assessments become valuable. Through tiny incisions, your doctor can inspect the uterus, fallopian tubes, ovaries, and surrounding tissues. If a problem is identified, treatment can often be done in the same procedure.
Laparoscopy is both a diagnostic and therapeutic tool, which is why it is so helpful for couples facing unexplained or persistent fertility challenges.
How Laparoscopy Helps in Diagnosing Fertility Problems
There are several fertility-related issues that can be accurately diagnosed through laparoscopy. These include:
• Endometriosis
• Blocked fallopian tubes
• Pelvic adhesions
• Fibroids
• Ovarian cysts
• Pelvic inflammatory disease
• Congenital abnormalities of the reproductive organs
These conditions may interfere with egg release, fertilisation, implantation, or overall reproductive function. Identifying them early can prevent delays in treatment and improve success rates naturally or through assisted methods.
Laparoscopy for Blocked Tubes: A Common Reason for Infertility
Fallopian tube issues are one of the most common causes of unexplained infertility. The fallopian tubes are essential because they are where the egg and sperm meet and where fertilisation happens. If a tube is blocked, the egg cannot travel properly, making conception difficult.
Laparoscopy for blocked tubes allows your doctor to see the exact location and severity of the blockage. Adhesions, infection, inflammation, and previous surgeries can all cause tubal blockages. During the same procedure, your doctor can attempt to open or clear the tubes if possible.
Mild blockages often respond well to laparoscopic correction. More severe cases may require IVF, but having an accurate diagnosis helps you make the right decision for your fertility plan.
Endometriosis Laparoscopy: A Key Step in Improving Fertility
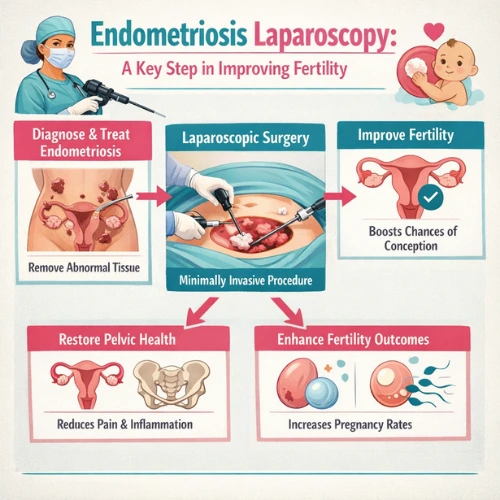
Endometriosis is a condition where tissue similar to the uterine lining grows outside the uterus. It can remain undiagnosed for years because symptoms vary widely. Many women with endometriosis struggle with fertility without realising the underlying cause.
An endometriosis laparoscopy helps your doctor identify and remove endometriosis lesions, cysts, and adhesions. Treating endometriosis surgically often improves pelvic health, reduces pain, and increases the chances of natural conception.
Restoring normal pelvic anatomy through surgery helps the ovaries and fallopian tubes function more efficiently.
How Laparoscopy Treats Fertility-Impacting Conditions
One of the biggest benefits of laparoscopy is that diagnosis and treatment can happen in the same procedure. Your doctor can:
• Remove adhesions
• Treat or drain ovarian cysts
• Remove small fibroids that interfere with fertility
• Open blocked fallopian tubes
• Excise endometriosis patches
• Correct structural abnormalities
These treatments restore normal pelvic anatomy and create a healthier environment for the reproductive organs. This improves natural conception rates and enhances the success of treatments such as IUI and IVF.
Benefits of Laparoscopic Surgery for Fertility
Women often prefer laparoscopy because of the significant advantages it offers.
1. Minimally Invasive
Small incisions mean less scarring and a gentler recovery.
2. Shorter Recovery Time
Most women return to normal activities sooner, which allows them to continue their fertility plans without major interruption.
3. Reduced Pain
The minimally invasive technique results in less postoperative discomfort.
4. Accurate Diagnosis
Laparoscopy provides a clear view of the pelvic organs, allowing precise identification of issues.
5. Immediate Treatment
Many problems can be treated during the same procedure, reducing the need for additional surgeries.
6. Improved Fertility Outcomes
Restoring pelvic health gives you a better chance of conceiving naturally or through assisted fertility methods.
Fertility Laparoscopy Success: What to Expect
Success rates vary depending on age, reproductive health, and the underlying condition being treated. Here is how laparoscopy improves fertility outcomes:
Treating Endometriosis
Removing endometriosis often increases the likelihood of natural conception within the following year.
Opening Blocked Tubes
Correcting mild to moderate tubal blockages can restore natural fertility.
Removing Adhesions
Adhesions can cause organs to stick together or move abnormally. Removal improves reproductive function.
Treating Cysts and Fibroids
Removing cysts or fibroids that interfere with conception improves ovulation and implantation.
Enhancing Assisted Fertility
Women preparing for IUI or IVF often have better outcomes after treating structural issues laparoscopically.
Laparoscopy does not guarantee pregnancy, but it creates a healthier environment for conception and removes barriers that might otherwise prevent success.
When to Consider Laparoscopy

You may consider laparoscopy if:
• You have been trying to conceive for a year or more
• Your ultrasound results are unclear
• You experience chronic pelvic pain
• You have symptoms of endometriosis
• There is a suspected tubal blockage
• You have had pelvic infections previously
• You have a history of abdominal surgery
Your doctor will recommend this procedure when non-invasive tests are not giving enough information or when symptoms point toward a structural issue.
Preparing for Laparoscopy
Preparation usually includes blood tests, imaging, and a preoperative evaluation. Share any symptoms you have, especially painful periods, pain during intercourse, or irregular cycles. This helps ensure all concerns are addressed during the procedure.
Recovery After Laparoscopy
Recovery is generally smooth. Most women return home the same day and resume daily activities within a week.
You may experience:
• Mild abdominal discomfort
• Bloating from the gas used during surgery
• Shoulder tip pain
• Light spotting
These symptoms usually settle within a few days.
Follow-up appointments are important so your doctor can explain the findings and guide your next steps.
How Laparoscopy Fits into Your Fertility Plan
Laparoscopy is often a turning point for many women. It provides clear answers, treats underlying issues, and strengthens your next steps. After the procedure, your doctor will help you decide whether to try naturally, proceed with IUI, or plan for IVF.
Understanding how laparoscopy supports fertility allows you to take an active role in your reproductive journey.
Conclusion
Laparoscopic surgery for fertility can bring valuable answers and treatment when you are searching for clarity. If you would like to explore whether laparoscopy can help your fertility journey, you can meet Dr. Neha at Prime Hospital in Dubai. Book a consultation to understand your options and move forward with confidence.