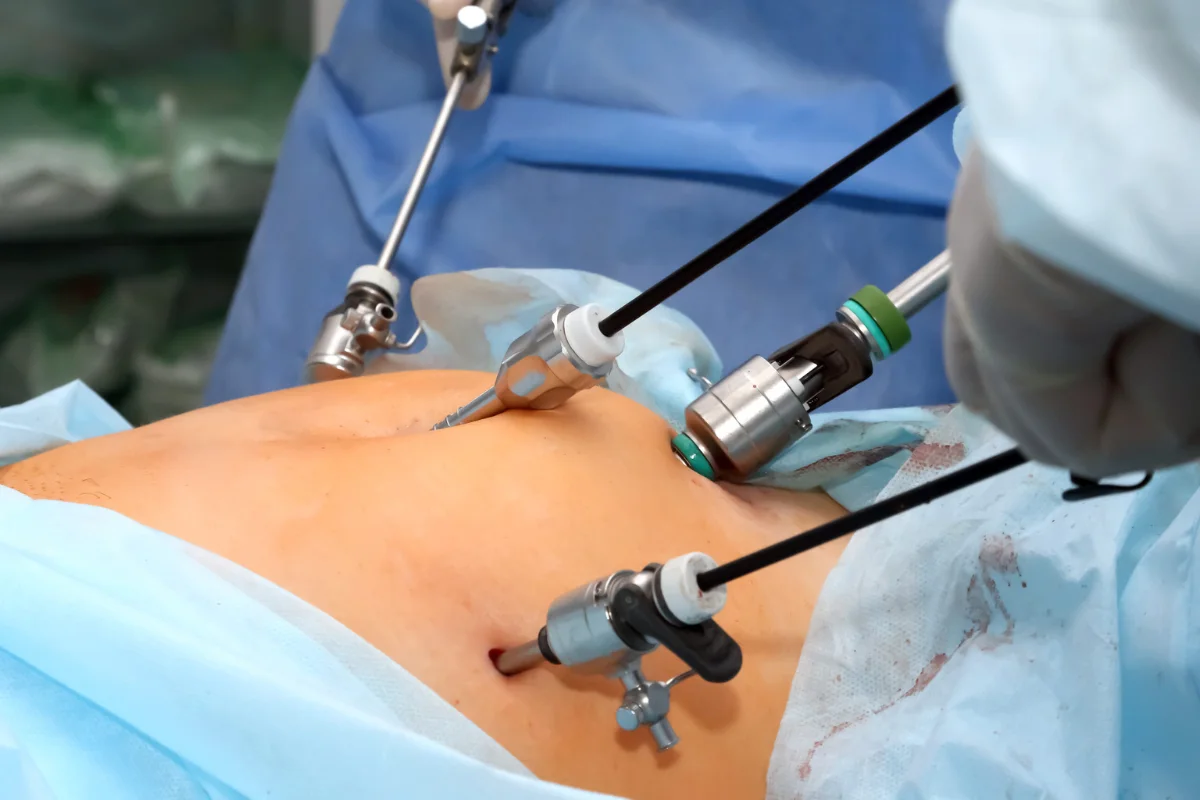
A total laparoscopic hysterectomy is a keyhole procedure used to remove the uterus, and in many cases the cervix, through small incisions in the abdomen. It is usually recommended when symptoms such as heavy menstrual bleeding, fibroids, adenomyosis, or severe endometriosis are significantly affecting quality of life and other treatments have not provided lasting relief.
For many women, this procedure offers a definitive solution to ongoing symptoms, with less pain, smaller scars, and a smoother recovery compared to open surgery.
A total laparoscopic hysterectomy is a minimally invasive surgery in which the uterus is removed using a laparoscope and specialised instruments passed through small cuts in the abdomen. The surgeon operates while viewing the pelvic organs on a high-definition screen, allowing the procedure to be performed with precision.
This approach is often chosen instead of open abdominal surgery because it usually allows for faster recovery, less blood loss, and a shorter hospital stay. Depending on the condition being treated, Dr. Neha Lalla will also discuss whether the ovaries or fallopian tubes need any additional treatment or removal.
The procedure is considered when preserving the uterus is no longer the best option for symptom control or long-term health.
A total laparoscopic hysterectomy may be recommended for women who have:
It is usually considered after a proper evaluation of symptoms, scan findings, age, medical history, and future reproductive plans.
Before surgery, Dr. Neha Lalla will review your symptoms, investigations, treatment history, and overall health in detail. This discussion is important to confirm whether hysterectomy is the right option, whether less invasive alternatives have been explored, and what the surgery is expected to improve.
You may be advised to undergo blood tests, imaging, and pre-anaesthetic assessment before the procedure.
The surgery is performed under general anaesthesia. Small incisions are made on the abdomen, and a laparoscope is inserted to visualise the uterus and surrounding pelvic organs. The uterus is carefully separated from its attachments and removed using a minimally invasive technique.
If needed, associated issues such as adhesions or endometriosis may also be addressed during the same procedure, depending on the surgical plan.
Most women stay in the hospital for a short period after surgery, depending on their recovery and the complexity of the case. Mild pain, fatigue, bloating, and light vaginal spotting can occur in the first few days. Recovery guidance, activity advice, and follow-up instructions are explained clearly before discharge.
Most women gradually return to normal routine over the following few weeks, though complete internal healing takes longer.
For women struggling with heavy bleeding, fibroids, adenomyosis, or severe endometriosis, this procedure can offer long-term symptom relief.
Because the surgery is performed through small incisions, recovery is usually easier than with open abdominal surgery.
The cuts used for laparoscopic surgery are much smaller, which means less visible scarring.
Many women experience less pain after laparoscopic hysterectomy compared to traditional open surgery.
Most patients are able to resume day-to-day activities sooner than they would after open surgery, depending on the extent of the procedure.
A minimally invasive approach often means a shorter hospital stay and earlier mobilisation after surgery.
If you are dealing with heavy bleeding, fibroids, adenomyosis, or severe endometriosis and want to understand whether surgery is the right option, Dr. Neha Lalla offers careful assessment and a clear, personalised treatment plan.
Dr. Neha Lalla is a Specialist Obstetrician and Gynaecologist in Dubai with over 16 years of experience in women’s healthcare.