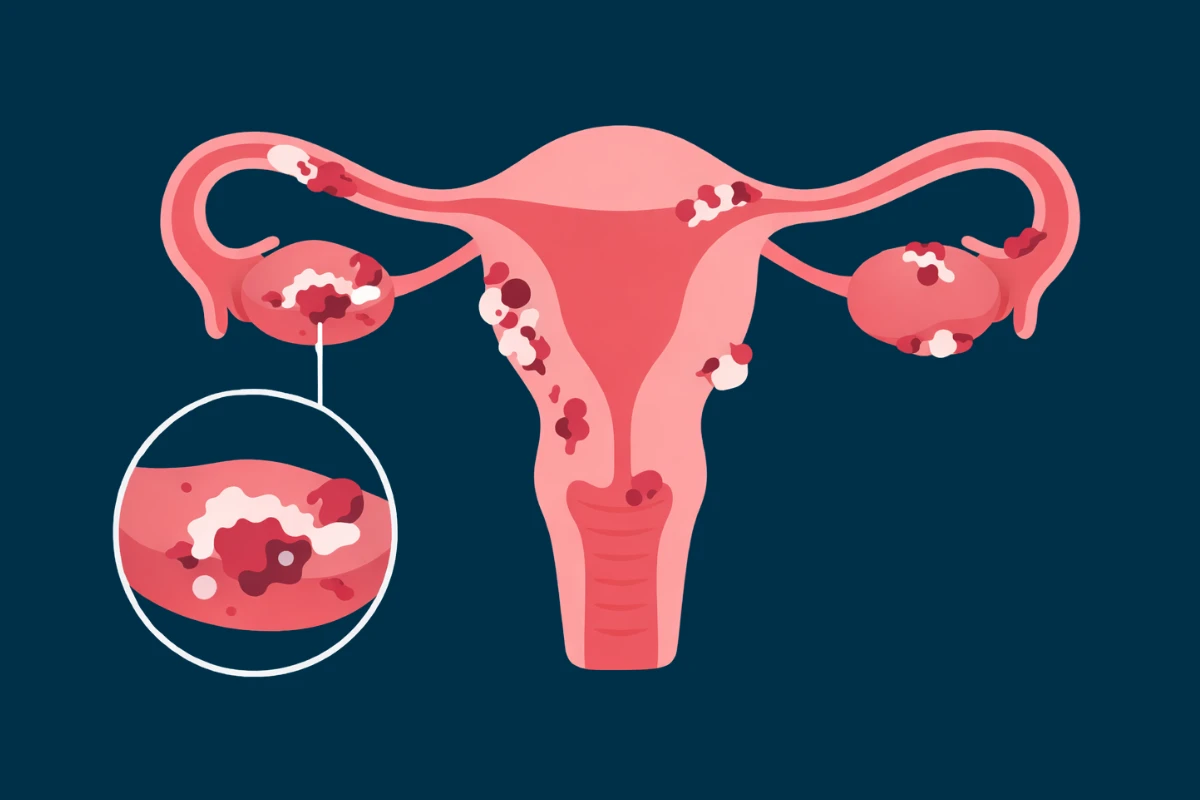
Endometriosis can affect fertility in different ways. In some women, it changes the pelvic environment, affects the ovaries or fallopian tubes, or causes adhesions that make conception more difficult. In others, the effect is less obvious, and the question becomes whether endometriosis is part of the reason pregnancy is not happening.
That is why endometriosis and fertility need to be looked at together, not as two separate concerns. If you are trying to conceive and also dealing with painful periods, an endometrioma, previous endometriosis diagnosis, or unexplained infertility, the right approach is one that considers both symptom control and reproductive goals at the same time.
Dr. Neha Lalla offers fertility-focused endometriosis care in Dubai with a clear, structured approach based on your symptoms, scan findings, ovarian health, and pregnancy plans.
Endometriosis and fertility care is the evaluation and treatment of endometriosis in women who are planning pregnancy or finding it difficult to conceive. The goal is not just to confirm the diagnosis, but to understand how the condition may be affecting fertility and what the most sensible next step should be.
Endometriosis can affect fertility by causing inflammation, pelvic adhesions, ovarian cysts known as endometriomas, distortion of pelvic anatomy, or reduced tubal function in some women. At the same time, not every woman with endometriosis will need surgery, and not every woman with infertility and endometriosis has the same treatment path.
This is why the management has to be individualised. The right plan depends on your age, symptoms, ovarian reserve, severity of disease, scan findings, and how long you have been trying to conceive.
This type of fertility-focused care may be helpful for women who have:
Some women come in with a diagnosis of endometriosis already. Others come in because pregnancy is not happening, and the evaluation starts to point in that direction. Both need a careful and fertility-conscious plan.
The first step is understanding the full picture. Dr. Neha Lalla will review your menstrual symptoms, fertility history, how long you have been trying to conceive, previous scans, ovarian findings, prior surgery, and any other factors that may be affecting fertility.
This part is important because the treatment decision is not based on endometriosis alone. It is based on how much it is affecting your fertility now.
Depending on your symptoms and reports, evaluation may include ultrasound, review of previous imaging, hormonal assessment, and fertility workup. If an endometrioma is present, or if there are signs that endometriosis is affecting the tubes, ovaries, or pelvic anatomy, that becomes an important part of planning.
In some women, laparoscopy may be considered when the diagnosis remains unclear, pain is significant, or surgery is likely to improve the fertility pathway.
Treatment depends on what endometriosis is doing in your case. Some women need monitoring and cycle-based fertility planning. Others may benefit from medical guidance, timed conception planning, or surgery to treat endometriosis, adhesions, or endometriomas in selected cases.
If surgery is being considered, the decision has to balance symptom relief with fertility preservation. The aim is not simply to remove disease, but to do so in a way that supports the best possible reproductive outcome.
Once the extent of endometriosis and its likely impact on fertility are clearer, the next step can be planned more confidently. That may mean trying naturally for a period of time, proceeding with fertility treatment, or treating the endometriosis surgically before moving forward.
This type of care looks at the whole picture, not just the endometriosis and not just the infertility in isolation.
For some women, endometriosis is a major factor. For others, it is only one part of the picture. Proper evaluation helps make that distinction.
When fertility matters, timing matters as well. A structured plan helps avoid unnecessary delay.
This is especially important in women with endometriomas or previous endometriosis surgery, where ovarian preservation needs careful consideration.
When endometriosis is affecting the ovaries, tubes, or pelvic anatomy, treatment may help improve the conditions for conception.
One of the biggest benefits is knowing what to do next, whether that is trying naturally, considering surgery, or moving ahead with fertility treatment.
If you have endometriosis and are trying to conceive, or you are starting to wonder whether it may be affecting your fertility, Dr. Neha Lalla offers careful evaluation and treatment planning tailored to both your symptoms and your pregnancy goals.
With endometriosis, the right fertility plan is the one that sees the full picture clearly.
Dr. Neha Lalla is a Specialist Obstetrician and Gynaecologist in Dubai with over 16 years of experience in women’s healthcare.